The government has announced that specialist doctors will be able to prescribe cannabis-based medicines but it remains to be seen if the new system will be any better than the ‘expert panel’. The evidence suggests not – while it was the expert panel that rejected the application this month of Eddie Braun, a three-year old who suffers with severe epilepsy, his neurologist – ie a specialist – was partly to blame.
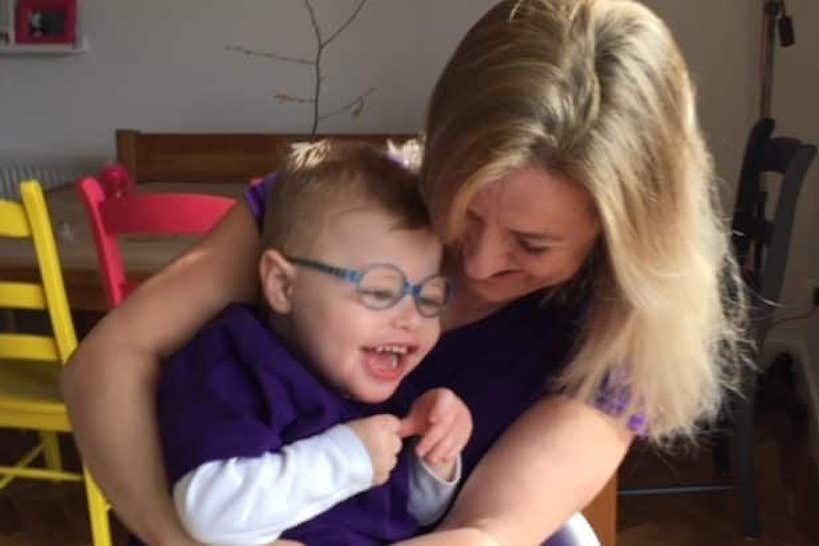
Eddie suffered with up to 500 seizures a day until cannabis oil bought over the counter reduced this to around 120 a day. But the benefits have plateaued and Eddie’s paediatric consultant applied to the panel for Tilray 2:100.
However, the panel said Eddie must try Epidiolex, which is similar to what he has already tried. Eddie needs a higher level of THC though.
In the UK, cannabidiol is legal and is available in high-street stores but the THC content must be below 0.2%, whereas in the medicine applied for it is 1%.
Eddie’s mother Ilmarie now feels as if the panel was set up to “pay lip service” to the families of seriously ill children.
She told the i: “We are disappointed, drained and tired. It’s been made out that medicinal cannabis will be more accessible than it is in reality. The Government are paying lip service. “Eddie cannot walk, talk or sit up independently and will suffer more brain damage if we can’t get his epilepsy better under control. We are desperate to give him a fighting chance.”
The Brauns are among a handful of parents who have applied for a licence. So far Billy Caldwell, 13, Alfie Dingley, six, and Sophia Gibson, seven, who all have severe epilepsy, have been allowed one.
Ilmarie, 42, from Chester, Cheshire, said the application is so “difficult and restrictive” that she believes very few will be accepted. She says she feels “fobbed off” for having been told to try yet another lower strength cannabis product. “To grant the application, we need to show that we are have tried all other medicines that could help, which we have.”

The panel seems to be willing to consider higher doses of THC only when it can be proven that it has been tried successfully in another country. But even if the family did this there is the worry that they would be turned down again for not trying Epidiolex first.
“For children like Eddie the risk of THC – taken at one per cent – is not higher than the risk of the damage their epilepsy can cause them. “Individual cases are not being weighed up and I feel they are convinced THC is just dangerous for children so what is the point in applying? “Eddie has not met his milestones and is screaming like a baby because he can’t communicate if he’s hungry or thirsty for example. It’s incredibly hard to see your child like that and feel so helpless.”
Another issue for families is being able to get the backing of doctors. All applications need the backing of the patient’s doctor and hospital trust – but many are fearful of taking on the clinical liability. “In Eddie’s case, the panel has questioned why his neurologist has not given his backing. The application has been supported by his paediatrician.
“I had a meeting with Home Office minister Nick Hurd who announced the formation of the panel who assured me the backing of Eddie’s paediatrician would be sufficient. “We had written to Eddie’s neurologist but he hasn’t responded. It doesn’t seem like the panel is interpreting the rules in the way they were intended to be.”
Ilmarie posted an impassioned and detailed Facebook post about the “confusing” process, shared below:
Earlier this month, Tannine Clarry, whose four-year-old daughter Indie has Dravet syndrome, also hit out at the expert panel for failing children.
Follow the UKCSC on social media: Facebook – Instagram – Twitter – Reddit